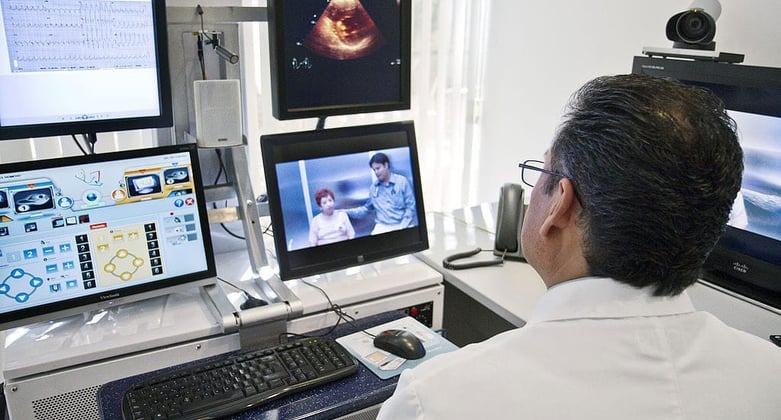
Telemedicine—allowing health-care providers to treat patients remotely via new technology—is gaining momentum as many states have passed laws allowing telemedicine along with updated practice standards, and more and more insurance companies, including Medicare and Medicaid, are offering coverage in certain situations.
The UMHS Endeavour explores the pro and cons of telemedicine, a new law in New Jersey and updates on coverage by Medicare. We will look at information from such sources as Berkeley Wellness, the American Telemedicine Association, Health Care Law Today, Medicare.gov and others.
Pros & Cons of Telemedicine
For now, telemedicine is primarily geared toward patients in rural areas with limited access to Primary Care doctors. Nothing will ever replace the value of an in-person doctor visit, but telemedicine is convenient and helps fill the gaps in the doctor shortage, especially in remote areas. BerkeleyWellness.com, the renowned health and wellness website at the University of California, listed the positive and negative aspects of telemedicine in a November 10, 2015 post “Is Telemedicine Right for You?”.
Berkeley Wellness gave the following examples of things that can be done with telemedicine:
- “You can send a digital image of a suspicious rash, along with your medical history, to a dermatologist, who will review it, diagnose, and prescribe medication to treat it.”
- “You can check-in with your doctor after surgery for follow-up care in your own home.”
- “If you have diabetes, you can monitor your blood sugar levels at home and upload the readings to your doctor's computer, saving yourself a time-consuming visit. Irregular blood sugar levels would generate an alert to the doctor's staff to call you in for immediate intervention to prevent complications.”
- “If you have hypertension, you can wear a monitor that tracks your blood pressure daily and transmits your results to your medical record, allowing your doctor to track your progress.”
Berkeley Wellness noted that while telemedicine offers unique benefits such as lower costs than in-person visits and the opportunity to get a second opinion on an MRI, X-ray and other scans and tests, there are numerous negative aspects. Some of the downsides include an “inadequate assessment” of a patient because the visit is done remotely and can result in an improper diagnosis. Critics say telemedicine is also more impersonal than an in-office visit and patients might be less likely to mention other issues that could be helpful to the doctor. In addition, technical problems with Internet connections can disrupt sessions.
Medicare to Start Telemedicine Coverage in January 2018
Medicare will start covering patients with chronic health conditions starting January 1, 2018, according to a news release from the American Telemedicine Association. The benefit will be called “remote patient monitoring” for patients with certain chronic health conditions. This will be in addition to traditional doctor visits and check-ups in clinics.
“Seniors with complex medical conditions will be benefit greatly from Medicare’s decision,” Sabrina Smith, Interim Chair of the American Telemedicine Association, said in the release. “As we have seen, frequent medical monitoring appointments can be quite challenging, particularly for those older adults who may be frail and unable to travel long distances.”
New Jersey Passes Telemedicine Law
New Jersey passed a telemedicine law that went into effect on July 21, 2017 after a year-long debate in the New Jersey Legistlature. The law, outlined on the website Health Care Law Today, explains exactly what can be covered in the state for New Jersey Medicaid, Medicaid managed care, and other state-funded health programs.
The law specifically defines telemedicine as a way to “bridge the gap between a health care provider who is located at a distant site and a patient who is located at an originating site,” and notes that telemedicine doesn’t include “audio only” telephone conversations, e-mail or fax communication.
The website says telehealth is “defined as the use of information and communications technologies, including telephones, remote patient monitoring devices, or other electronic means, to support clinical health care, provider consultation, patient and professional health-related education, public health, health administration, and other services.”
The law notes that health-care providers, in addition to licensed physicians, may include nurse practitioners, nurses, clinical social workers, and others.
Patients are not required to go through an in-office exam with the health-care provider before an telemedicine appointment, but the provider must look over the patient’s medical history and records prior to the electronic visit. If the patient doesn’t have a regular Primary Care provider, the health-care provider can refer the patient to someone.
What Will Medicare Cover for Telemedicine?
The Medicare.gov website notes Medicare Part B (for people age 65 and older) covers what they call “telehealth” under the following conditions:
- “Using an interactive 2-way telecommunications system (with real-time audio and video)
- By a doctor or certain other health care provider who isn’t at your location.”
Medicare Part B covers patients in rural areas under certain conditions and only the patient is located at one of the following:
- A doctor's office
- A hospital
- A critical access hospital (CAH)
- A rural health clinic
- A federally qualified health center
- A hospital-based or critical access hospital-based dialysis facility
- A skilled nursing facility
- A community mental health center
Many private health plans cover telemedicine. Patients are advised to contact their insurance company for details.
About UMHS:
Built in the tradition of the best US universities, the University of Medicine and Health Sciences focuses on individual student attention, maintaining small class sizes and recruiting high-quality faculty. We call this unique approach, “personalized medical education,” and it’s what has led to our unprecedented 96% student retention rate, and outstanding residency placements across the US and Canada. UMHS is challenging everything you thought you knew about Caribbean medical schools.

Scott is Director of Digital Content & Alumni Communications Liaison at UMHS and editor of the UMHS Endeavour blog. When he's not writing about UMHS students, faculty, events, public health, alumni and UMHS research, he writes and edits Broadway theater reviews for a website he publishes in New York City, StageZine.com.